2000, 106: 393-402.ĭe Groot LJ: Dangerous dogmas in medicine: the nonthyroidal illness syndrome. Nagaya T, Fujieda M, Otsuka G, Yang J-P, Okamoto T, Seo H: A potential role of activated NF-κB in the pathogenesis of euthyroid sick syndrome. Iltumur K, Olmez G, Ariturk Z, Taskesen T, Toprak N: Clinical investigation: thyroid function test abnormalities in cardiac arrest associated with acute coronary syndrome. 
1982, 3: 164-217.īianco AC, Salvatore D, Gereben B, Berry MJ, Larsen PR: Biochemistry, cellular and molecular biology, and physiological roles of the iodothyronine selenodeiodinases. Wartofsky L, Burman KD: Alterations in thyroid function in patients with systemic illness: the 'euthyroid sick syndrome'. Although the traditional approach is to not treat the euthyroid sick syndrome with levothyroxine because it will all be shunted into rT 3, the authors ask whether we should consider treating cardiac patients who have the euthyroid sick syndrome with T 3 (and not T 4) to facilitate cardiac recovery. If reverse T 3 is high, then what these authors are describing is truly the euthyroid sick syndrome. If it were truly a simple deficit in T 3 production, reverse T 3 should also be low. This could be differentiated from the euthyroid sick syndrome by measuring reverse T 3 levels. 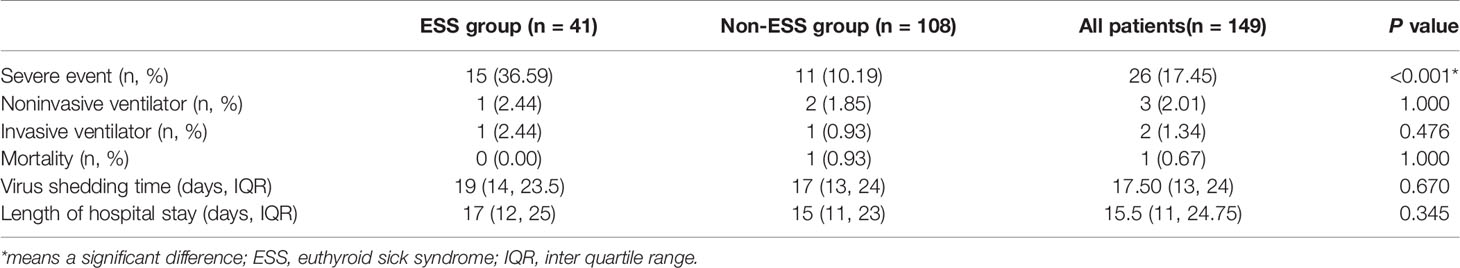
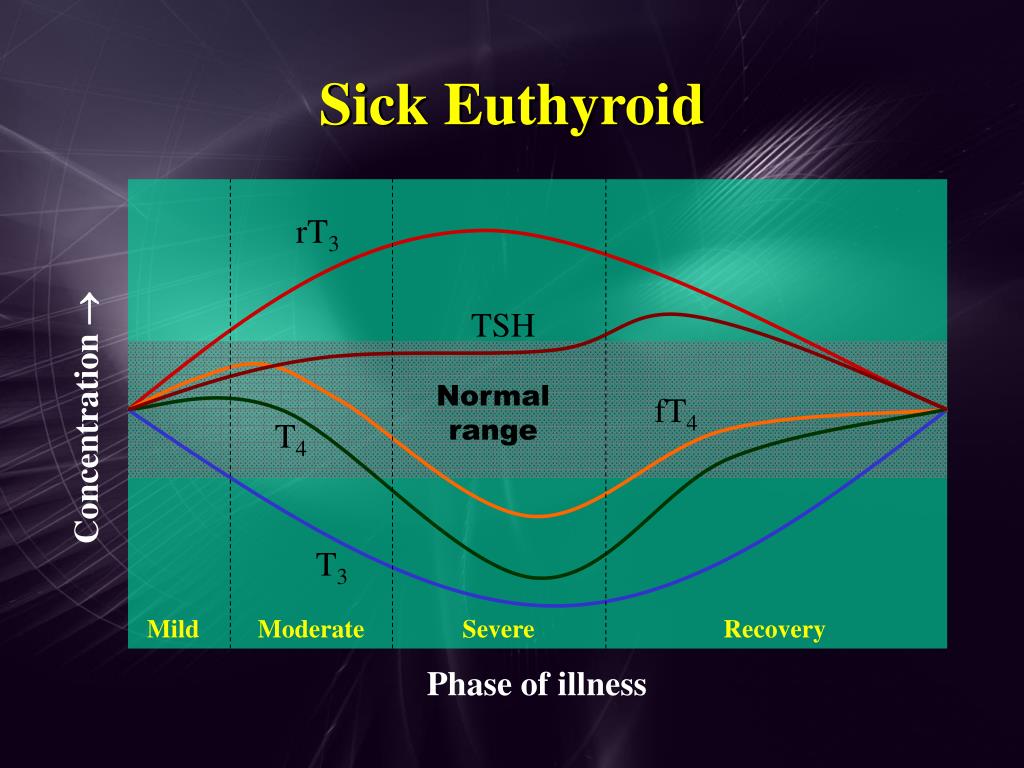
If this is a true 'low T 3 syndrome' due to hypothalamic–pituitary ischemia, combination T 4/T 3 therapy might be of value during the period of decreased production. This study of patients with acute cardiac illness is of interest because the authors are proposing that as we are able to resuscitate many of these acutely ill patients they will then have increased T 4 requirements, and the 'low T 3 syndrome' might actually hinder our efforts. Because one does not know what phase of recovery a patient has reached, we have focused on maintaining the T 4, which is the 'storage form' of the hormone, in the normal range. Thus, as they recover from the acute illness they seem, transiently, to have a form of primary hypothyroidism. It is very possible that the higher TSH level represents recovery manifested as an asynchronous return of the hypothalamic–pituitary and thyroid axes to normal. Critically ill patients with the euthyroid sick syndrome can have a very low TSH level or it can be as high as 20 μIU/ml. This raises an interesting question of whether the level of TSH, either in itself or in how it changes over the illness, has any prognostic information. Cytokines can also contribute to the suppression of TSH. Cytokines, including IL-6, IL-1, and tumor necrosis factor-α, contribute to the suppression of the 5' deiodinase, thus shunting T 4 into rT 3. They do mention the more likely etiology, which is cytokine-mediated suppression of T 3 production. Unfortunately, they initially try to create an argument that the acute episode was associated with relative hypotension to the hypothalamic–pituitary axis leading to a 'low T 3 syndrome', although they are not able to offer any proof that such ischemia occurs in their cohort. The body responds to illness by shunting T 4 disproportionately towards rT 3, which cannot be converted to the biologically active form of T 3 but only deiodinated to T 2.Īlthough this process makes sense teleologically as a form of conservation of energy, these authors raise the question of whether this could actually impair the body's response to the acute illness, namely the myocardial ischemia. Normally, about 40% of secreted T 4 is monodeiodinated in the 5' position to yield T 3, and a similar fraction is monodeiodinated in the 5 position to yield rT 3. T 4 is normally metabolized through sequential deiodination to T 3 then to 3,3'-di-iodothyronine (T 2), which is then rapidly degraded to monoiodothyronines and thyronine. The physiologic changes that lead to these alterations are the body's attempt to conserve metabolism during illness. Analysis of such patients led to the recognition of the euthyroid sick syndrome, which is characterized by low normal thyroxine (T 4) levels, low normal 3,5,3'-tri-iodothyronine (T 3) levels, variable thyroid-stimulating hormone (TSH) levels and elevated 3,3',5'-tri-iodothyronine (reverse T 3 rT 3) levels. The question of whether thyroid hormone supplementation should be provided to critically ill patients without a known history of thyroid disease is not a new debate. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
